Gardasil 9
In the fight against the Human Papillomavirus (HPV), Gardasil 9 stands tall as a powerful vaccine offering protection against a range of diseases. This comprehensive guide delves into the key aspects of Gardasil 9, from dosage and administration to its effectiveness and safety, providing essential insights to help you make informed decisions about this critical preventive measure.
| Dosage form | |
|---|---|
| Manufacturer | |
| Origin | |
| Pack size | |
| Generic Name (Ingredient) | Proteins of HPV Types 6, 11, 16, 18, 31, 33, 45, 52, and 58, amorphous aluminum hydroxyphosphate sulfate, yeast protein, sodium chloride, L-histidine, polysorbate 80, sodium borate, and water for injectio |
| Potency | 10 Single-dose 0.5 mL Vials |
Assuming your emergency circumstances for this product, visit Urgent Quotation page. Besides, for any pharmaceutical questions, please ask us in the comments section.
Description
Gardasil 9 is an advanced vaccine specifically designed to protect against certain diseases caused by HPV. This protective shield is available for girls and women aged 9 through 45 years, as well as boys and men in the same age range.
Dosage and Method
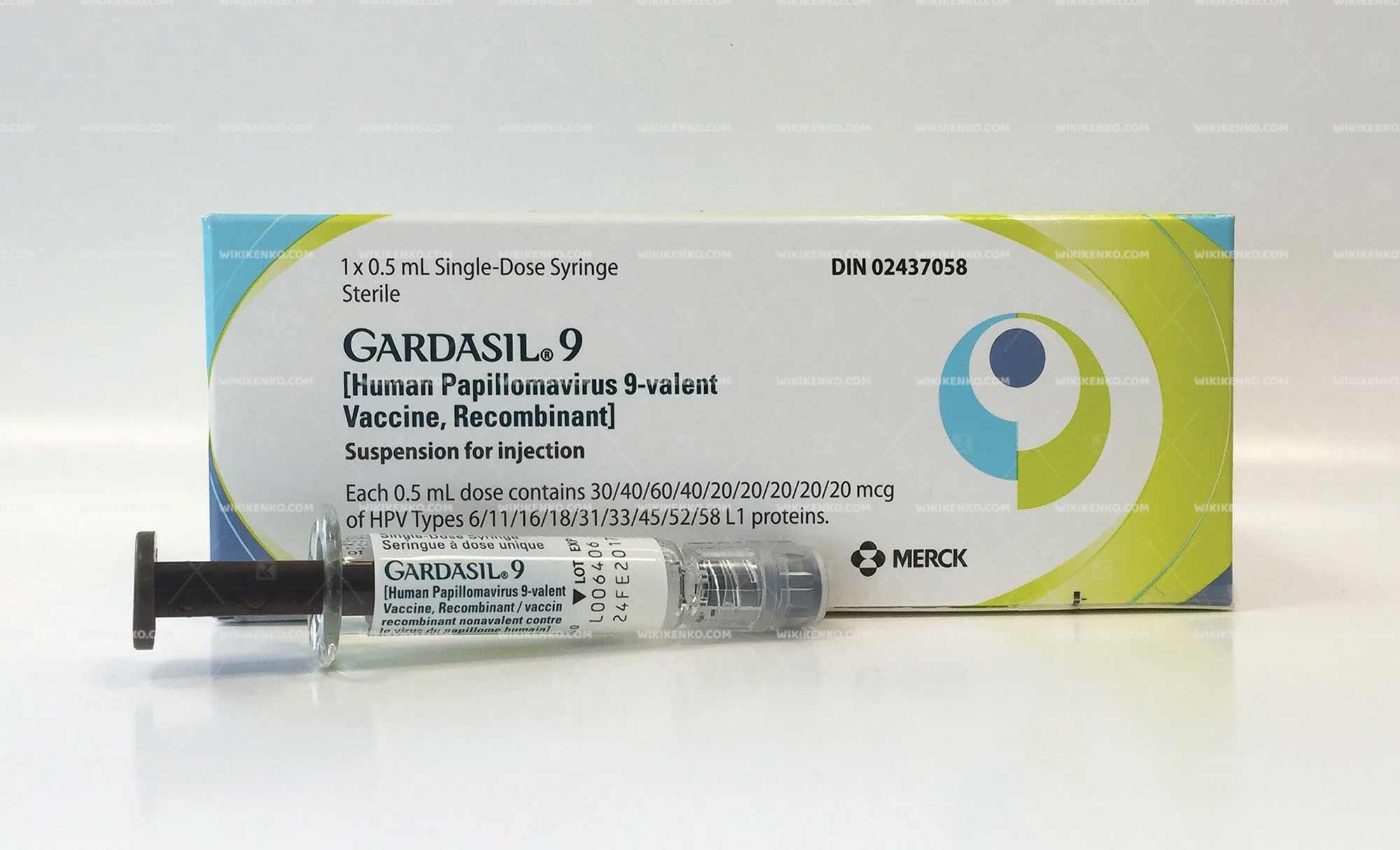
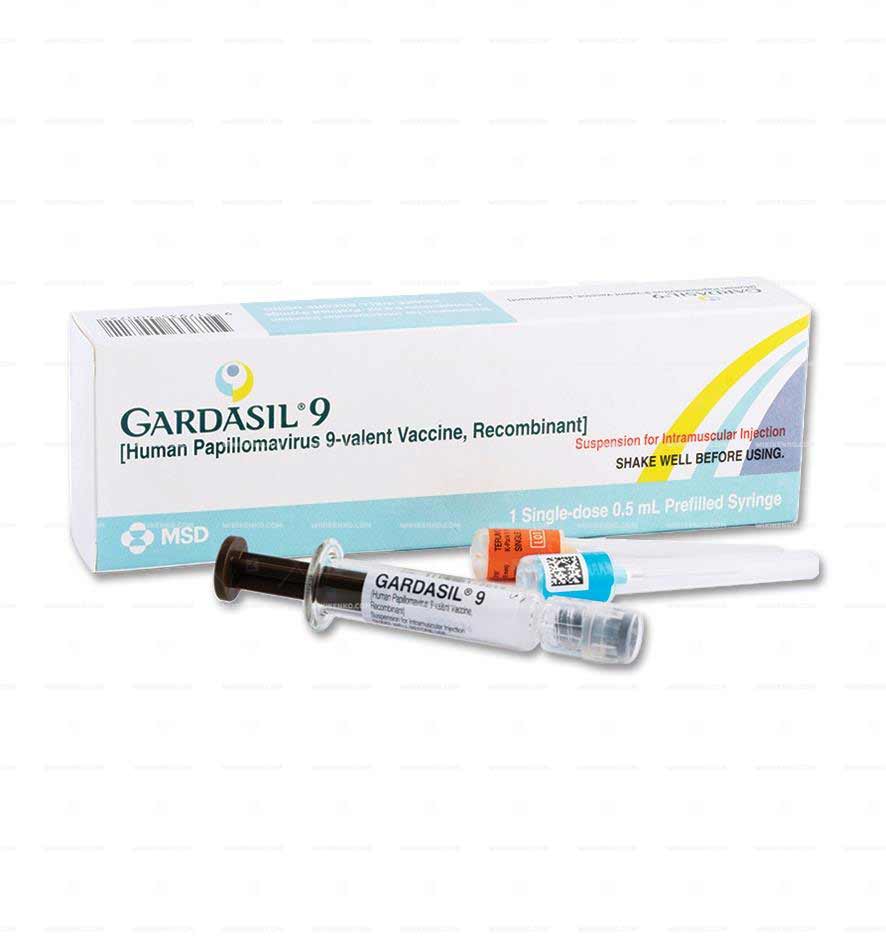
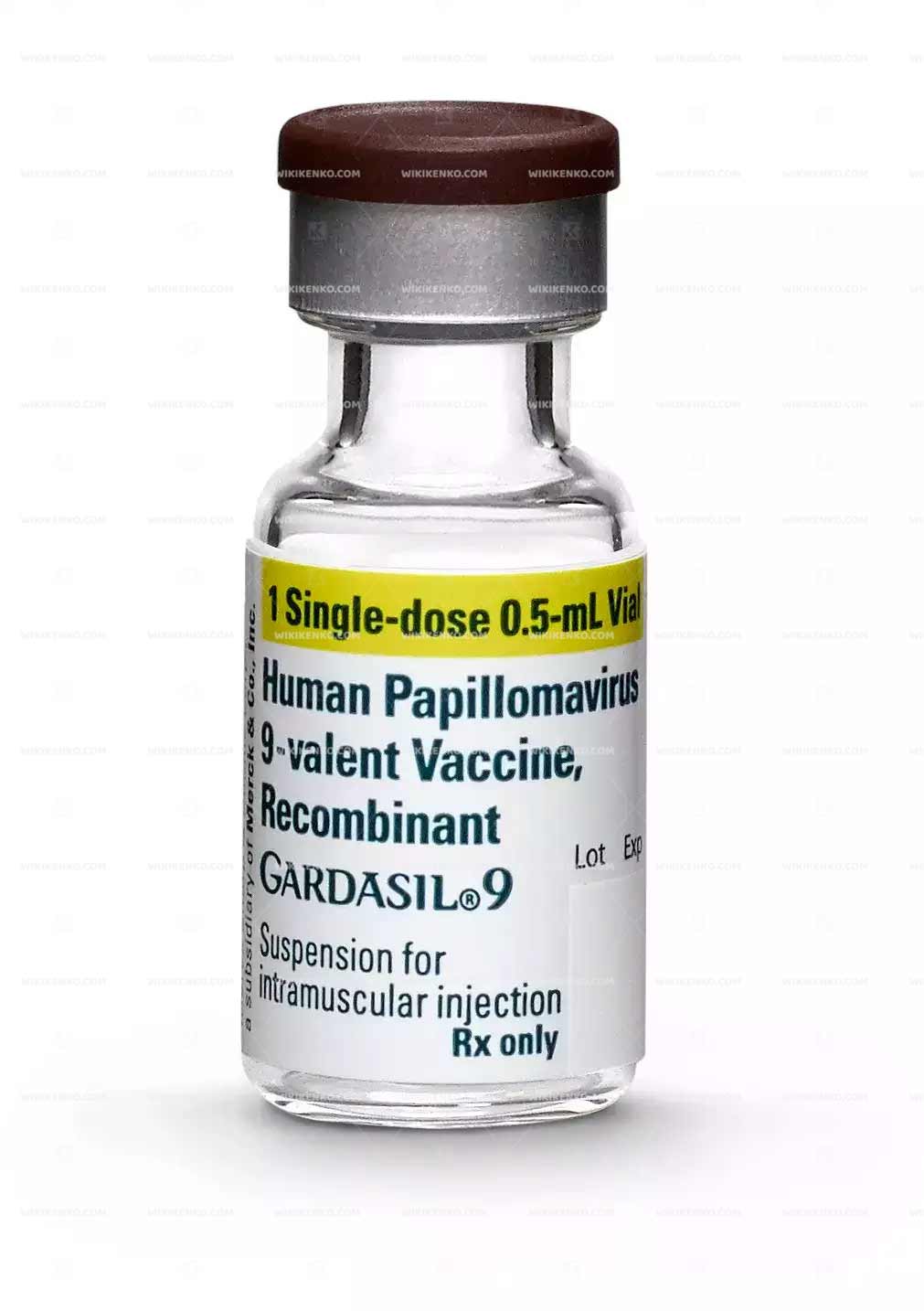
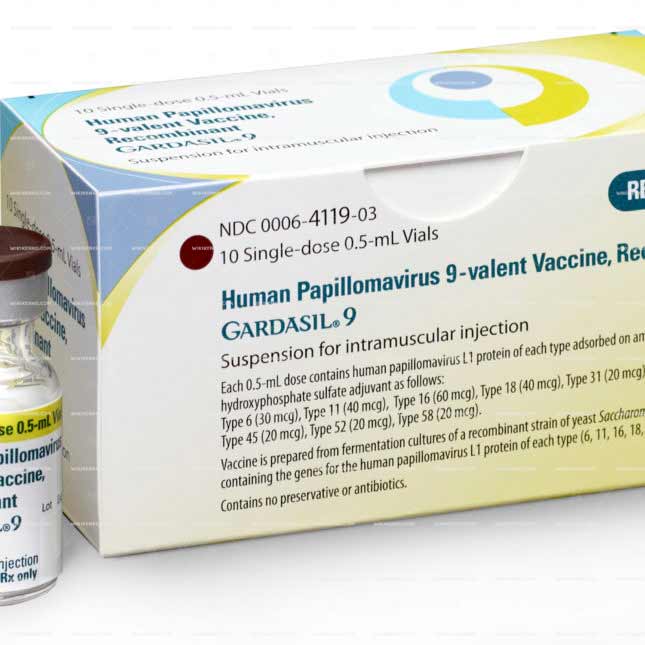
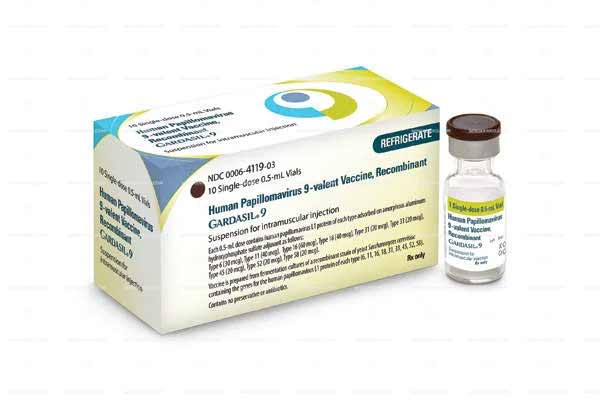
Gardasil 9 comes in the form of a suspension for injection, available in vials or prefilled syringes. The vaccine is typically administered according to either a two-dose or three-dose schedule, depending on the recipient’s age group.
For males and females aged 9 to 14 years, a two-dose schedule is recommended, with the second dose administered between five and thirteen months after the first dose. On the other hand, for those aged 15 years and over, as well as females aged 9 to 14 years opting for the three-dose schedule, the second dose should be given two months after the first, and the third dose four months after the second. Notably, there should be a minimum of one month between the first and second doses and at least three months between the second and third doses. It’s crucial to ensure that all doses are administered within a year.
Individuals who receive the first dose of Gardasil 9 are strongly advised to complete the full dosing regimen using this vaccine.
Method of Administration
Gardasil 9 is specifically designed for intramuscular use and should be administered in the deltoid region of the upper arm or the higher anterolateral area of the thigh. As with any vaccine, there is a slight risk of syncope (fainting) following administration. As a precaution, recipients are advised to be observed for 15 minutes after receiving the vaccine.
Indications and Usage
Gardasil 9 offers extensive protection against an array of HPV-related conditions. For girls and women, the vaccine is indicated for the prevention of cervical, vulvar, vaginal, anal, oropharyngeal, and other head and neck cancers caused by HPV types 16, 18, 31, 33, 45, 52, and 58. Additionally, it guards against cervical, vulvar, vaginal, and anal precancerous or dysplastic lesions caused by HPV types 6, 11, 16, and 18, as well as genital warts caused by types 6 and 11.
For boys and men, Gardasil 9 effectively prevents anal cancer caused by HPV types 16, 18, 31, 33, 45, 52, and 58, along with anal precancerous or dysplastic lesions caused by types 6, 11, 16, and 18. It also offers protection against genital warts caused by types 6 and 11. Notably, certain head and neck cancers, such as throat and back of mouth cancers, caused by the HPV types mentioned above, are also within the protective range of Gardasil 9.
Limitations
While Gardasil 9 is a potent preventive tool, it’s important to be aware of its limitations. Vaccination with Gardasil 9 does not eliminate the need for women to continue undergoing recommended cervical cancer screening. Similarly, recipients should not discontinue anal cancer screening if advised by their healthcare provider. Gardasil 9 has not been proven to offer protection against diseases from vaccine and non-vaccine HPV types to which an individual may have been previously exposed through sexual activity.
Additionally, Gardasil 9 is not intended for treating active external genital lesions or cancers. The vaccine does not provide protection against diseases caused by HPV types not included in its formulation.
Side Effects of Gardasil 9
Like any medication, Gardasil 9 may cause side effects, but they are typically mild and transient. Common side effects include mild pain, redness, itching, or swelling at the injection site. Some individuals may experience headaches, which generally subside quickly.
Less common side effects may include fever, nausea, and joint or muscle pain. In rare cases, people may develop an itchy red rash (hives), and extremely rarely, difficulty breathing and airway restriction may occur.
It’s essential to remember that these side effects are typically mild and self-limiting, resolving within a few days. However, if you experience persistent or concerning side effects, promptly seek advice from your healthcare provider.
Pregnancy and Breastfeeding
According to the Centers for Disease Control and Prevention (CDC), the HPV vaccine is not recommended for use during pregnancy. If a person is pregnant, the initiation of the vaccination series should be delayed until after the pregnancy. Notably, pregnancy testing before vaccination is unnecessary.
For individuals who identify a pregnancy before completing the full HPV vaccine series, the CDC recommends waiting until after pregnancy to finish the vaccine series. The good news is that Gardasil 9 is noninfectious and does not contain a live virus, making it of low concern for pregnancy. As for breastfeeding, there is limited information on the use of Gardasil 9 during this period. It’s always prudent to discuss any concerns with your healthcare provider for personalized guidance.
Contraindications and Precautions
The Centers for Disease Control and Prevention (CDC) have outlined specific contraindications and precautions for the HPV vaccine. Individuals with a severe allergic reaction (e.g., anaphylaxis) to a vaccine component or following a previous dose of an HPV vaccine should not receive Gardasil 9. Furthermore, Gardasil 9 is contraindicated for persons with a history of immediate hypersensitivity to yeast, as it is produced in Saccharomyces cerevisiae (baker’s yeast).
Receiving the vaccine during a moderate or severe acute illness is a precaution, and vaccination should be deferred until symptoms of the acute illness improve.
Effectiveness of Gardasil 9
Gardasil 9 has been extensively studied, and the trials leading to its approval demonstrated its near 100% effectiveness in preventing cervical, vulvar, and vaginal infections and precancers caused by all seven cancer-causing HPV types it targets. The 9-valent vaccine boasts an impressive efficacy rate of 96.7%.
As with all HPV vaccines, it’s essential to highlight that vaccination with Gardasil 9 does not eliminate the need for women to continue recommended cervical cancer screening. Similarly, recipients should not discontinue anal cancer screening if advised by a healthcare provider.
Different HPV Vaccines
Currently, three HPV vaccines are available: Cervarix, Gardasil, and Gardasil 9. Each offers protection against specific HPV types. Cervarix is a bivalent vaccine targeting HPV types 16 and 18, responsible for 70% of cervical cancers. Gardasil, a quadrivalent vaccine, protects against the same two types as Cervarix, in addition to HPV types 6 and 11, which account for 90% of genital warts.
Gardasil 9, the most comprehensive among the three, provides protection against the four HPV types included in Gardasil, along with an additional five types (31, 33, 45, 52, and 58) causing about 15% of cervical cancers.
Conclusion
With Gardasil 9 standing as a highly effective shield against the devastating impact of HPV-related diseases, it is crucial to make informed decisions about vaccination. Discussing your specific needs and circumstances with your healthcare provider will enable you to embark on a proactive journey towards safeguarding your health.
Empower yourself and your loved ones with the knowledge to make the right choices. Make HPV prevention a priority, and together, we can combat the threat of HPV-related diseases.
Use the form below to report an error
Please answer the questions as thoroughly and accurately as possible. Your answers will help us better understand what kind of mistakes happen, why and where they happen, and in the end the purpose is to build a better archive to guide researchers and professionals around the world.
The information on this page is not intended to be a substitute for professional medical advice, diagnosis, or treatment. always seek the advice for your physician or another qualified health provider with any questions you may have regarding a medical condition. Always remember to
- Ask your own doctor for medical advice.
- Names, brands, and dosage may differ between countries.
- When not feeling well, or experiencing side effects always contact your own doctor.
Cyberchondria
The truth is that when we’re sick, or worried about getting sick, the internet won’t help.
According to Wikipedia, cyberchondria is a mental disorder consisting in the desire to independently make a diagnosis based on the symptoms of diseases described on Internet sites.
Why you can't look for symptoms on the Internet
If diagnoses could be made simply from a textbook or an article on a website, we would all be doctors and treat ourselves. Nothing can replace the experience and knowledge of specially trained people. As in any field, in medicine there are unscrupulous specialists, differences of opinion, inaccurate diagnoses and incorrect test results.


Reviews
There are no reviews yet.